A very, very dark place’: Hospitals brace for crisis-care mode with too many patients, not enough staff
Ken AlltuckerUSA TODAY0:190:49https://imasdk.googleapis.com/js/core/bridge3.427.1_en.html#goog_1634236857
COVID-19 deaths and hospitalizations are at record levels, and the rising case toll from Americans’ holiday travel has created an unprecedented surge with no relief in sight.
The problem is especially ominous in the nation’s intensive care units – specialized units crowded with a record number of critically ill Americans as the nation struggles through the most dangerous phase of the pandemic.
On Thursday, California announced stay-at-home orders for regions where intensive care units are nearly full. A growing chorus of medical experts say hospitals and states must prepare to shift to crisis-care mode, a designation with standards for hospitals to navigate life-and-death decisions when they become overwhelmed.
Crisis standards mean hospitals with too many patients and not enough staff likely will need to triage patients, prioritizing care to those mostly likely to benefit when demand outstrips resources.
New York hospitals struggled to adapt to staff and equipment shortages during the deadly spring months. And although hospitals now have more drugs, equipment and expertise, strained medical staffs could limit the number of Americans who get timely care.
“What we see now is just the beginning of the post-Thanksgiving peak,” said Eric Toner, senior scholar with the Johns Hopkins Center for Health Security. “It’s going to be huge, and it’s going to be awful.”
Of the 100,667 hospitalized with COVID-19 as of Thursday, 19,442 were in ICUs – the largest number of critically ill patients since the pandemic began, according to COVID Tracking Project figures. More than 267,000 Americans have died, including 2,879 on Thursday – a new daily record.
U.S. Centers for Disease Control and Prevention Director Robert Redfield said this week that deaths could reach 450,000 by February.On Friday, the agency released a summary of public health recommendations to reduce spread of the coronavirus, such as masking and avoiding nonessential indoor places. Get the Coronavirus Watch newsletter in your inbox.
Stay safe and informed with updates on the spread of the coronavirusDelivery: VariesYour Email
Our neighbors, our family members’:Small-town hospitals overwhelmed by COVID-19 deaths
Hospitals already are employing strategies to stretch resources. Utah hospitals have canceled surgeries and shifted staff to makeshift ICU units to care for the growing number of COVID-19 patients. North Dakota’s rural hospitals, short on available beds and expertise, in recent weeks transferred patients to surrounding states. And in Colorado, Gov. Jared Polis signed an executive order authorizing the state health department to order at-capacity hospitals to halt admissions and transfer patients.
In the spring, when New York City became the epicenter of the coronavirus pandemic, health care professionals flocked to the Big Apple to help besieged hospitals. But with a limited pool of nurses, doctors and respiratory therapists available for temporary gigs, experts say it’s unlikely hospitals will get meaningful relief from out-of-state practitioners.
Toner said the nation’s stretched health care workforce is “our most critical scarce resource.”
“We have ventilators. We’re doing better with PPE and supplies,” he said. “But we have no way to significantly expand our staffing.”
That is what worries public health officials. The next three months will be “the most difficult time in the public health history of our nation,” Redfield said.
Last week, Johns Hopkins published an extensive study of New York City’s hospitals during the pandemic. The study, led by Toner with input from 15 ICU directors, described gut-wrenching choices, such as when to extend or end life-sustaining care for patients.
The Association of American Medical Colleges this week urged medical schools, hospitals and states to plan or implement crisis standards to battle the latest surge – expected to be the most widespread and deadly of the pandemic.
“We’re now up to about 100,000 a day in the hospital,” said Janis Orlowski, Association of American Medical Colleges’ chief health care officer. And, “this is just the start.”UK to receive first vaccine supply; NYC elementary students return to class – virus updatesHis father died alone in a nursing home. The obit he wrote calls out anti-maskers.Low flu vaccine rates hurdle for COVID-19 vaccineGet the latest news straight to your phone: Download the USA TODAY app
The strain on caregivers
New Mexico’s ICU beds were at 103% capacity as of Thursday, the highest rate in the nation, according to U.S. Department of Health and Human Services figures.
Space also is tight at the state’s medical-surgical units in Albuquerque, Las Cruces and Farmington, and rural hospitals are quickly filling, too, according to Troy Clark, president and CEO of New Mexico Hospital Association. https://bbc91d2e5af312e591f5a4afea579382.safeframe.googlesyndication.com/safeframe/1-0-37/html/container.html
Hospitals used extra space in emergency departments and operating rooms not licensed for bedsto accommodate patients, but Clark said the major bottleneck is finding enough doctors, nurses and respiratory therapists to care for them.
COVID-19’s effect on health care workers is far greater now than during the spring or summer. Hospital workers can be infected at home or in their communities. Even if they are not sick, workers exposed to the virus often wait up to four days for test results, Clark said.
“That’s where we’re stressed across the state of New Mexico right now,” he said. “While there may be physical beds, there is not a nurse, a nurse tech or respiratory therapist to care for those patients.”
Hospitals overwhelmed: Exhausted staffs, surging COVID-19 cases push nation’s limits
In North Dakota, Gov. Doug Burgum issued an order last month allowing staff who test positive for the virus but show no symptoms to keep caring for COVID-19 patients.
Other states are trying to fill shortages with contract employees who travel out of state for temporary jobs.
Competition is so fierce Clark estimates 70% of contract workers who commit start jobs at their preferred hospitals. With staffing agencies commanding salaries up to three times normal for these positions, there might be multiple lucrative offers for gig employees to choose.
When cases surged in June and July, travel nurses and other temporary workers with Banner Health, Arizona’s largest health provider, filled shifts. With cases again on the rise, the Phoenix-based health system hired 1,500 and is seeking another 900 contract workers, but Chief Clinical Officer Marjorie Bessel acknowledged it’s difficult.
Rhode Island opened two temporary field hospitals with a capacity of almost 1,000 beds to alleviate crowded conditions. Lifespan’s Rhode Island Hospital, which operates a 600-bed field hospital in Providence, hired temporary nurses, nursing assistants respiratory therapists and pharmacy technicians. The state’s hospitals are the fullest in the nation, with 88% occupancy, according to HHS.
“Our staffing issues are significant,” said Cathy Duquette, a Lifespan executive.
Hospitals coast to coast are facing similar staffing challenges, experts say.
“In the past, you could anticipate the cavalry coming,” AAMC’s Orlowski said.
Unlike past crisis situations when health care workers traveled to New Orleans after Hurricane Katrina or to New York this spring, doctors and nurses are needed close to home.
“Reinforcements from other parts of the country aren’t going to be possible now,” Toner said. “For the most part, hospitals will have to deal with the staffing they have.”
COVID-19 hospitalizations pass 100K in US: Experts fear weary staff will be ‘overrun’ by patients

Hospitals at a ‘very dark place’
Hospitals increasingly must stretch staffing to meet the realities of the surge.
In California, several hospitals have applied to loosen the state’s mandatory nurse-to-patient staffing ratios because of COVID-19-related patient increases and staffing shortages. Last week, Antelope Valley Hospital in Lancaster gained state approval to relax staffing ratios, drawing criticism from a nurses’ union that said the move put patients at risk.
But hospitals will continue to seek ways to stretch resources under crisis-care scenarios, experts say.
Nursing home residents who need to be hospitalized might find such stays are shortened, Orlowski said.
And when things get really tight, hospitals need to choose who gets life-sustaining therapies. A person with minor ailments might get treatment while a person with several preexisting conditions and low oxygen might not.
If doctors determine a person’s chances of death are significantly high, “they may say, you know what, we are going to use our resources not to do this miraculous save, but we’re going to concentrate our resources on people we know who will be improved by our care,” Orlowski said.
New York hospitals struggled with similar decisions when allocating ventilators and kidney dialysis for lifesaving care during the worst days this spring.
According to the Johns Hopkins report, some hospitals did not have clear written guidelines on ventilators when “capacity became limited.” Doctors had to decide whether to intubate, or insert breathing tubes into people, and which type of ventilator to use. In some cases, hospitals had the equipment but not enough staff.
The same was true for COVID-19 patients suffering kidney failure. Therapy was in short supply for these patients, so doctors had to triage, or choose whether kidney failure patients would get two or three days of dialysis, according to the Johns Hopkins report.
During the summer surge, Banner Health in Arizona faced a shortage of ECMO machines. Extracorporeal membrane oxygenation machines are a last-ditch therapy for those whose lungs are damaged and they can no longer effectively breathe with a ventilator. The machine pumps blood to an artificial lung, adds oxygen and returns the blood to the patient.
ECMO machines are limited sodoctors across several hospitals work together to try to maximize use of the therapy. But based on the trajectory of the surge in cases, Bessel said it’s “very likely” some won’t get access.
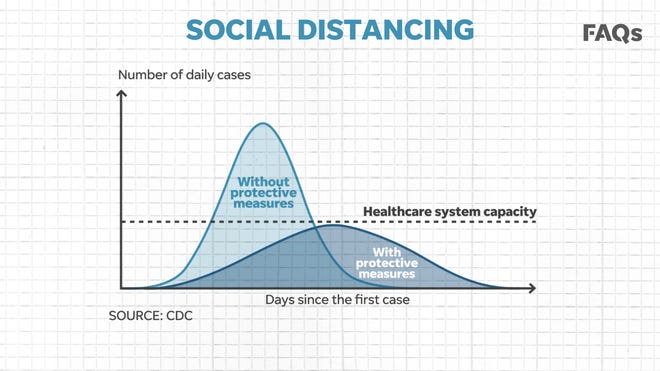
When the crisis worsens and if hospital must triage limited services, “it’s a very, very dark place to be for health care systems, for patients, for families,” Bessel said. “That’s why mitigation and other tactics right now are so important to try and flatten the curve to reduce the likelihood that we get to a point where we need to operate in such a fashion.”
Dr. Amesh Adalja, a senior scholar at Johns Hopkins Center for Health Security, said hospital administrators face tough choices.
“You have to think about capacity on a day by day basis, because we don’t see this surge ebbing any time soon.”
Ken Alltucker is on Twitter as @kalltucker or can be emailed at alltuck@usatoday.com